Table of Contents
This story contains descriptions of sexual assault.
Tara Velan lay on a heated table when she began to feel the hands of her massage therapist slide under the loosely draped sheet, to her growing alarm.
She’d found Johnnie Lopez, a Seattle massage therapist, on Groupon and had asked him to work on her back and neck. But now she felt frozen as Lopez groped her breasts, buttocks and inner thighs. They were alone in the office, and she feared what would happen if she tried to sit up and leave.
Velan didn’t know then, in July 2016, that Lopez was already under investigation by both the Washington state Department of Health and police for two similar complaints that had been filed by women in March and June.
“I am appalled that I was on the end of the timeline, that there were multiple [victims],” Velan said in an interview. “And yet I could find a Groupon for this person, just like it was nothing.”
The Washington state Department of Health suspended Lopez’s license nine months after receiving the first complaint. For Velan, the delay was devastating. But by DOH standards, it was a swift resolution.
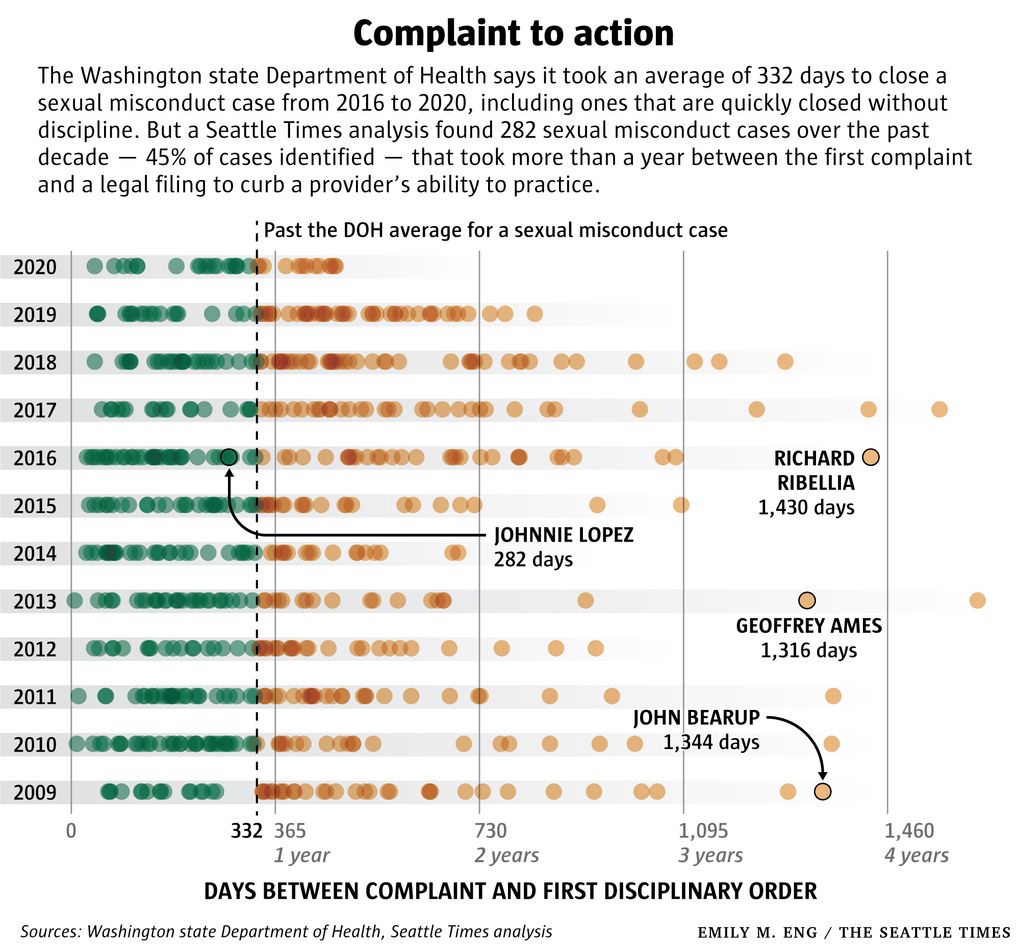
In 282 cases since 2009, state health regulators have taken more than a year to discipline a provider accused of sexual misconduct, an investigation by The Seattle Times has found.
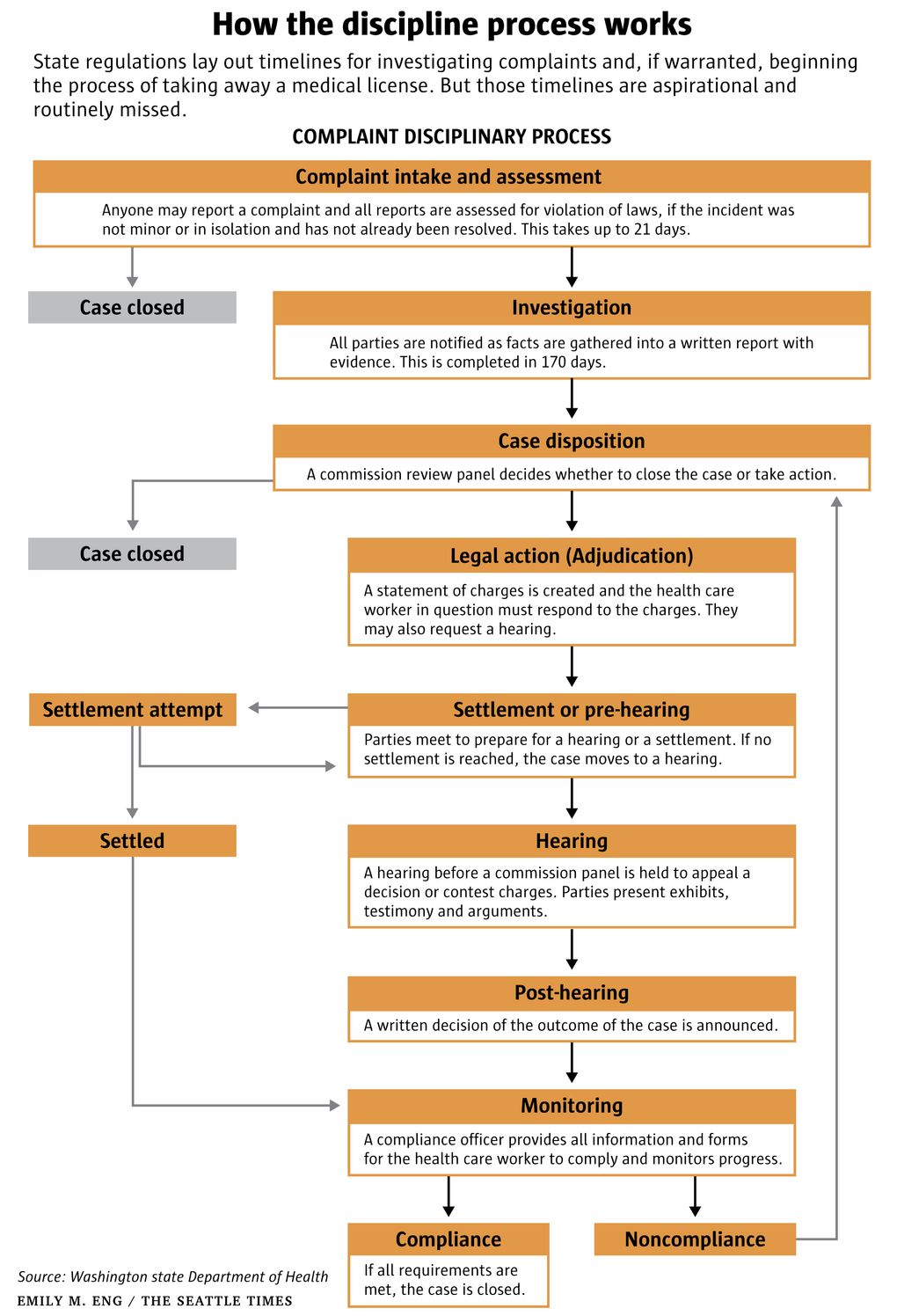
From the moment officials receive a complaint, they have deadlines laid out in state regulations: 21 days to evaluate the allegations, 170 days to investigate, 140 days to decide whether to bring charges, with more time limits to hold hearings. But these deadlines are largely aspirational and routinely missed.
Health care providers are increasingly contesting disciplinary charges rather than settling, a trend that is drawing out proceedings, according to state health commissions. At times, health officials themselves have busted deadlines trying to build a case.
For regulators, striking the balance is fraught: Act too quickly and risk unfairly casting a cloud over a provider or securing only minimal discipline; take too long gathering evidence and more patients could suffer harm.
Lengthy investigations can lead abusive providers to become more emboldened in their misconduct, said Azza AbuDagga, a health-services researcher for Public Citizen, a consumer advocacy organization. “Sexually abusive doctors tend to reoffend, they tend to have multiple victims,” she said.
Christie Spice, DOH’s acting assistant secretary over disciplinary cases, said the department doesn’t tolerate sexual misconduct and that the vast majority of providers have never had a complaint against them.
“But the disciplinary process isn’t perfect,” she said, adding that the accused also have rights. “Sometimes the process isn’t expeditious, but we work as hard as we can to protect the safety of patients.”
Cases lingering past regulatory deadlines are flagged for enhanced oversight, sometimes resulting in more staffing to expedite it, according to DOH.
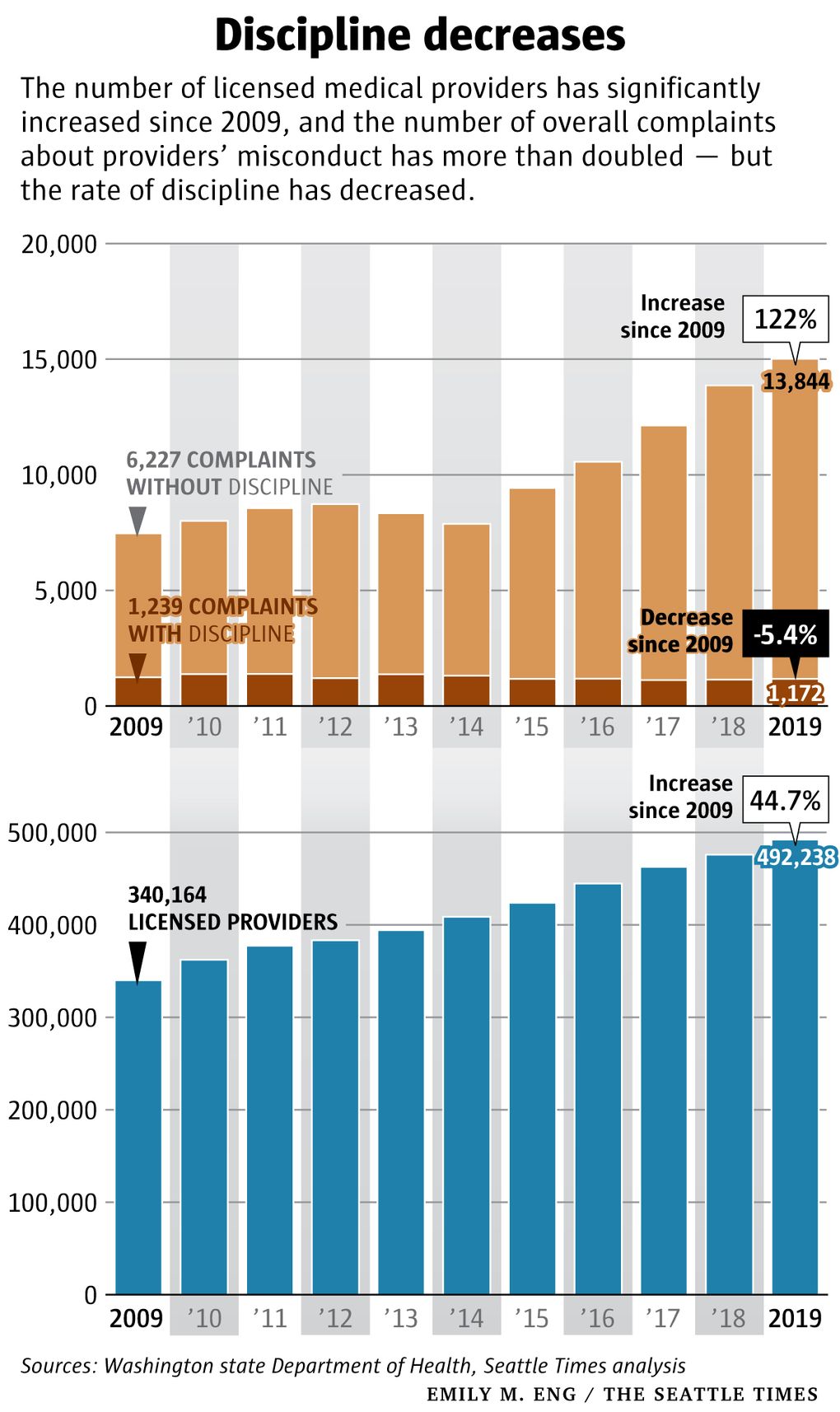
The number of complaints of all types against licensed providers more than doubled from 2009 to 2019, as the number of licensed health care professionals increased by 45%, to nearly 500,000.
But the number of complaints that resulted in discipline slightly declined over that time, according to a Times analysis of DOH data. Health officials said “staffing levels are not a consideration when (it) decides to pursue a case.”
In a series of written responses, DOH said it “looks at the merits of each complaint individually” and “does everything it can to swiftly gather the evidence needed to have a solid case against a licensee.”
DOH said it took an average of 332 days to resolve sexual misconduct cases from 2016 through 2020 — a calculation that includes complaints quickly closed because regulators found they didn’t warrant an investigation. It doesn’t reflect how long it takes to actually discipline a provider.
So The Times built its own data set of sexual misconduct disciplinary actions, reviewing thousands of pages of records DOH posted online and logging the dates when authorities first took action. Among 628 cases since 2009, the most actions were taken against massage therapists and nursing assistants, followed by doctors.
In nearly a third of the cases, disciplinary authorities took longer than the 332-day average cited by DOH — just to file charges or reach a settlement. One out of every 10 cases involved extraordinary delays — taking more than two years between the initial complaint and the first disciplinary action.
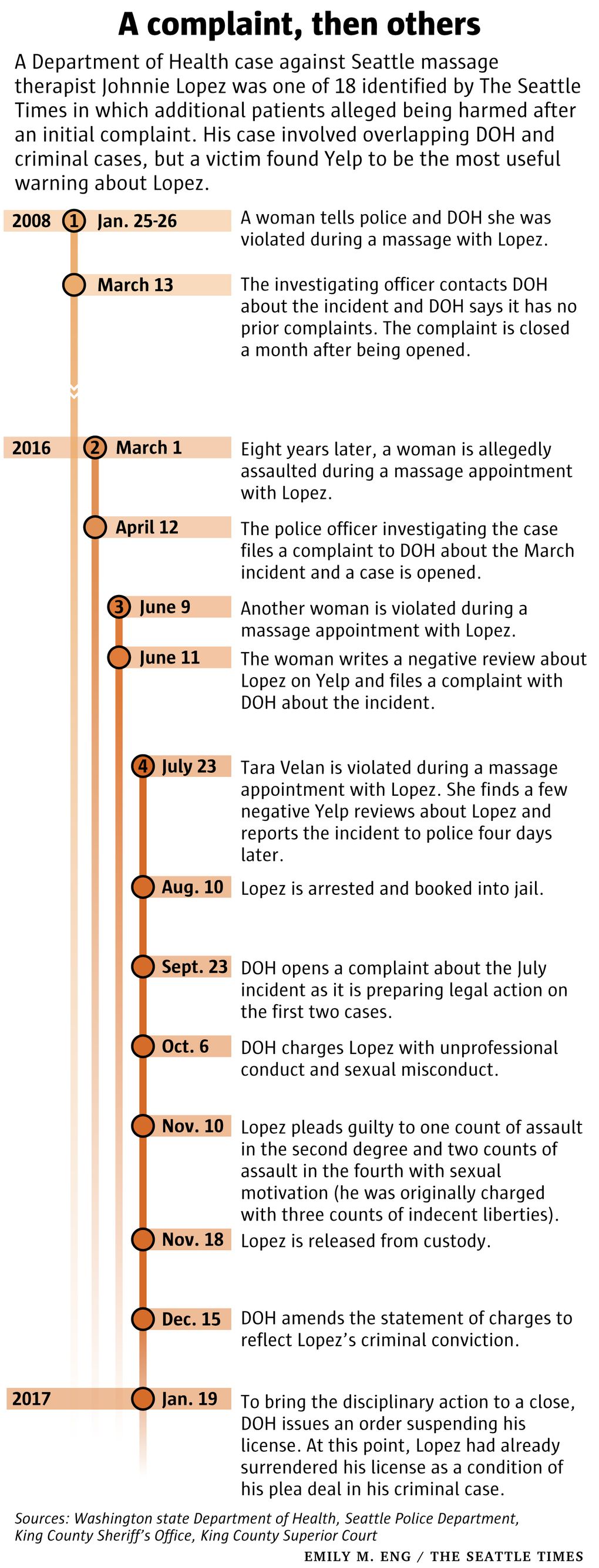
The Times found 18 cases, including Lopez’s, in which additional patients alleged being harmed by a health care provider after the department began investigating a complaint of sexual misconduct that ultimately resulted in disciplinary action.
“The details of these cases are absolutely upsetting, and our hearts go out to the victims,” Spice said. Sexual misconduct, she added, is a “huge priority” for DOH Secretary Dr. Umair Shah and he’s asked the department to look for ways to improve its disciplinary processes.
There is no easy way to compare the timeliness of medical discipline across states, and the Federation of State Medical Boards said it does not track the data nationally. For a benchmark — the rate of serious discipline against physicians — Washington ranked 29th among states, according to an analysis by Public Citizen in March.
Cases can exceed timelines for a host of reasons, DOH said. Witnesses and victims may be hard to track down or won’t cooperate. Law enforcement may ask DOH to wait, pending a criminal investigation. Expert witnesses may be needed. There is no limit to how many times disciplinary hearings can be postponed for scheduling reasons.
As a result, the first public sign of a provider’s misconduct sometimes emerges not from DOH but in online reviews, civil lawsuits and criminal charges — such as in Lopez’s case.
The department suspended Lopez’s license in January 2017, but by that time, he had already permanently surrendered his license as a condition of pleading guilty to assault.
Lopez did not respond to interview requests but sent a statement by email: “I feel bad that people felt uncomfortable despite my best efforts to communicate and provide professional care.”
Velan was angry after learning that others were harmed before her, but also understood the need for investigators to build a strong case. “How many people get away with this?” she said.
A legacy of delay
DOH’s struggles to investigate sexual misconduct allegations is not new: A 2006 investigation by The Seattle Times found the department did not investigate many sexual misconduct complaints, and enforced scant oversight and inconsistent discipline of providers named in the complaints. It prompted a state audit that found a backlog of complaints and lags in investigating them.
In response, state lawmakers in 2008 required the licensing boards and commissions — which regulate a range of medical providers — to refer some sexual misconduct complaints to DOH for expedited handling. DOH hired more staff in the years following the audit, and average case closure times decreased over the following decade, according to agency reports.
But sexual misconduct cases still take significantly longer to resolve on average than complaints overall, according to DOH. In one case, involving a physician assistant in Soap Lake named John Bearup, it took 1,344 days between the initial complaint and him permanently surrendering his license. Efforts to reach him were unsuccessful.
The first public sign of sexual misconduct by Geoffrey Ames, a Richland doctor, emerged in a lawsuit.
The suit, filed in 2014, accused Ames of having a sexual relationship with a patient and negligent care that led the woman to kill herself. The plaintiff — the woman’s surviving spouse — obtained text messages in which Ames talked about sleeping with the patient and described her as “the love of my life.” Ames testified he “made up” the messages but didn’t recall why.
Ames, representing himself in the lawsuit, denied responsibility for the patient’s death and said the spouse “is defaming me in front of the medical board, my patients and my family.” The suit settled after Ames filed for bankruptcy.
The state Medical Commission, which regulates doctors and physician assistants, charged Ames with misconduct and lying to its investigator in December 2015, nearly two years after the lawsuit made the claims public.
Between the first complaint and the charges, Ames prescribed excessive doses of a thyroid medication that led to another patient’s emergency hospitalization, according to disciplinary records. Nine months after filing charges, the commission revoked Ames’s license, entering a default order when he didn’t respond to charges.
Ames now goes by “Jake” and is a licensed physician in Mexico, where he pitches “potentially curative” cancer treatments on his website. “I work in a far better regulatory environment than the U.S. and other countries,” the site says. He didn’t respond to phone calls and emails seeking comment.
It isn’t clear that the medical commission knew about the lawsuit. Officials said they don’t search court records for a provider they’re investigating. The commission has “no knowledge of civil suits unless the litigants alert us,” it said in written responses to questions from The Times.
The commission said it gives “enhanced scrutiny” to sexual misconduct cases and that the Bearup and Ames cases were examples of “technically complex cases that required extensive investigation, legal negotiation, and eventually litigation.” In both cases, the commission said it had to hire expert witnesses, conduct additional investigations requested by state attorneys and that hearings were pushed back at the request of the practitioners.
Though the allegations of misconduct were severe in both cases, the medical commission didn’t exercise one of the most powerful tools at its disposal: immediately stopping a provider from practicing.
Even when authorities do summarily suspend a license, the speed of the disciplinary action depends on how long it takes authorities to decide a provider is a danger.
Accused of misconduct — and a crime
The woman’s late-night email to a DOH investigator didn’t mince words. “I feel that once an individual has crossed the line with one massage client,” she wrote in August 2018, “they most certainly will do so again to another. Perhaps with worse intentions.”
She was referring to Jeremy Wilson, a massage therapist in Whatcom County. And she was right — there would be more complaints to come, according to DOH records.
After five women complained to DOH or police that Wilson touched them sexually and pressed himself against them during massages, DOH announced in a November 2019 news release that it had “immediately suspended” his license.
The department didn’t advertise that it had received the initial complaint more than a year earlier, according to the criminal complaint and disciplinary records. It didn’t mention that Wilson had allegedly groped another patient after the initial complaint.
It also didn’t mention that one of his patients reported being harmed in May — after DOH filed charges — but before it summarily suspended his license in November.
Wilson has been charged with five felony counts of indecent liberties in Whatcom County, with a trial tentatively scheduled for February 2022. He didn’t respond to a letter and phone calls, and his lawyer did not respond to repeated requests for comment. DOH said the case remains active and declined to comment.
By contrast, it took just six days to suspend the license of a doctor accused of sexually assaulting a patient during a pelvic exam. The disciplinary process began after the doctor had been arrested — one of 20 cases resolved in less than two months that began with a law-enforcement investigation, The Times found.
“In cases where criminal action is involved, action is faster simply because the investigation is already completed by another entity,” the medical commission said in a statement.
But sometimes police involvement has the opposite effect.
“Neither DOH or law enforcement want to put a victim or a witness through both a criminal trial and an administrative hearing if it can be avoided,” the department wrote.
Yet that is what happened in the case of Joseph Price, a nursing assistant. He was charged with attempted rape and indecent liberties related to an alleged sexual assault of a co-worker, but was acquitted of the first charge in April 2018. The Clallam County prosecutor dropped the charge of indecent liberties after jurors deadlocked in two trials that stretched through October 2018.
Only then did DOH resume its own investigation of Price’s license, which had remained active through the trials. The department filed disciplinary charges against Price in January 2020, nearly three years after the complaint, and suspended his license for six years in June 2021.
“It was shocking that they would even suggest waiting until a trial was over,” said Price’s former co-worker, Sabrina Sisneros. She relived the ordeal by testifying in two trials and the subsequent DOH hearing. The department “took way too long,” Sisneros said.
In an interview, Price denied the allegations and said it didn’t make sense for the department to pursue them given he hadn’t been convicted. “Not guilty is not guilty,” he said.
Sexual misconduct cases can be especially contentious and often come down to a patient’s word against a provider’s, said Darrell Cochran, an attorney who has represented many plaintiffs in sexual abuse cases involving health care providers. In these cases, Cochran said, health care providers “get an incredible amount of protection from their position.”
Anatomy of a delay
When a police officer notified DOH of a complaint against Richard Ribellia, a Moses Lake chiropractor, health officials weren’t sure how to handle it.
A teenager told police in February 2016 that Ribellia exposed her breasts without warning and touched her genital area over her underwear while placing a protective X-ray shield, according to DOH records obtained by The Times in a public disclosure request.
The officer learned another patient alleged a similar experience with Ribellia. But the local prosecutor declined to file charges, citing his understaffed office and concern that an expert for the chiropractor could give a jury reasonable doubt he’d done anything wrong.
The situation would be “better handled” by DOH, the prosecutor wrote in a memo. Initially, DOH staff had some reservations.
“I’m not seeing enough here to say that either of the sexual misconduct rules were violated,” Patrick Hanley, a staff attorney, wrote to a board member of the Chiropractic Quality Assurance Commission, in an email.
The commission offered Ribellia an informal settlement in August 2016 but he rejected it, saying he’d done nothing wrong.
By the time the commission served Ribellia with formal charges in March 2018, it was 406 days behind schedule, case records show.
DOH “was building a solid case against the provider, ensuring we had the right evidence and securing expert witnesses,” the department said in a written response.
Then the real delays began.
A department legal assistant mistakenly emailed Ribellia’s attorneys an unredacted copy of Hanley’s legal analysis, triggering a legal tug of war that DOH ultimately won.
Ribellia changed lawyers. A new judge was assigned to the case. Disciplinary hearings were postponed at least four times. And as the commission continued to build its case, it received new allegations alleging similar conduct.
Ultimately, DOH’s charges cited 11 patients, although two said Ribellia’s treatment didn’t make them uncomfortable. The charges included two other patients who claimed they were harmed while DOH was gathering evidence, disciplinary records show.
The commission summarily suspended Ribellia’s license in January 2020, concluding after nearly four years that he presented an “immediate danger” to the public. It dropped the suspension the next month as too restrictive, and the litigation continued for a year and a half.
In August, the commission suspended Ribellia’s license for at least 42 months, a ruling that came 2,016 days after the initial complaint.
Colin Kearns, an attorney for Ribellia, said that he “continues to deny that anything he did was sexual misconduct” and has steadfastly contended his treatments were appropriate. Of his patients who testified against him, Kearns said, Ribellia “regrets that they feel anything he did was for anything other than appropriate care.”
The disciplinary case against Ribellia was among the longest reviewed by The Times, but such legal pushback from providers has been increasingly common.
The commissions overseeing doctors and physician assistants, chiropractors and nurses all asked the Legislature for a funding boost in the 2019-21 budget cycle, citing rising legal costs or rising numbers of complaints; they saw the requests mostly granted.
“The growing inability to investigate and take legal actions on cases in a timely manner does not protect the public,” the Nursing Care Quality Assurance Commission wrote, requesting an additional $3.2 million to counter a trend of fewer cases completing on time amid a surge in complaints.
“Mad as hell”
For the public, DOH’s online database of providers only shows a disciplinary record if they have been formally charged or agreed to an informal settlement. There is no public trace of an initial sexual misconduct complaint against Lopez, the massage therapist — eight years before he pleaded guilty to assaulting patients.
Police launched an investigation in 2008 of the complaint filed by a woman named Cheryl, who requested her last name not be used for fear of retaliation. She told authorities she was assaulted during a massage and notified DOH two days later. Prosecutors declined to file charges due to what they said was “insufficient evidence.” DOH didn’t find a violation, records show.
“I’m mad as hell,” Cheryl told The Times. She felt that had she not been the only woman at the time to allege harm, her case would have risen to a higher priority. Had Lopez been charged, she said, “there may not have been this happening eight years later.”
For Tara Velan, it only occurred to her after her assault to search for other complaints about Lopez online. And there, on Yelp, she found two negative reviews posted within days of each other in June 2016 — barely a month before her massage. One post warned other women to avoid him.
The author of the review wrote it two days after her own massage, using a different name to protect her identity, and also filed a complaint directly with DOH.
The woman works in health care so she was familiar with the complaint process. The quickest way to warn others, she told The Times, was to post a review on Yelp.






More Stories
Does Urgent Care Do Blood Work?
A Bridge to Stronger Couples Relationships for the Latino Community
5 Effective Strategies for Migraine Management