Hundreds of health care workers at Cox Medical Center in Branson, Missouri will soon be equipped with personal panic buttons, following a year of increased violence against staff members. The coronavirus pandemic, the medical center said, has “greatly” contributed to the number of assaults.
The panic buttons will be provided to 300 to 400 staff members working in “high risk areas” of the hospital — including emergency and inpatient hospital rooms — and are expected to be implemented by the end of the year.
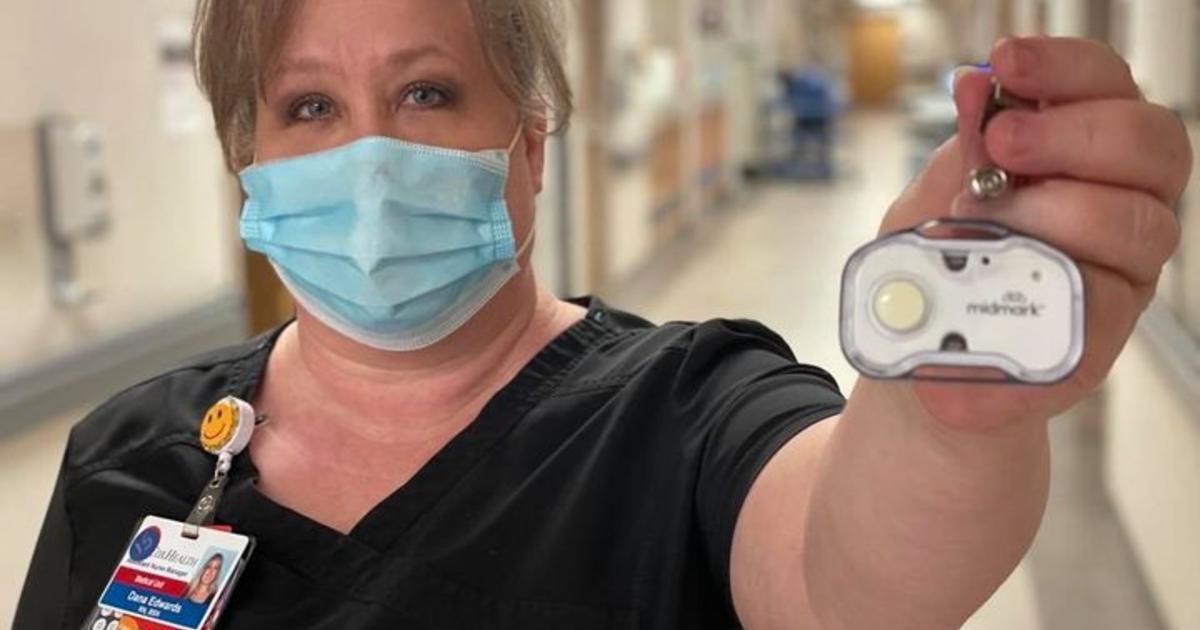
If a worker experiences distress, they can press the button — which is attached to their badge — to activate a personal tracing system, notify security, and deploy a pop-up alert on hospital computers to show the employee’s location. If the button is pressed from inside a room, a light pattern will flash outside of that room and a tone will be played at designated nurse call consoles, the medical center said.
The panic buttons were trialed at the facility last year.
CoxHealth received a $132,000 grant for the panic buttons earlier this month from the Skaggs Foundation, a Branson-based non-profit that helps develop philanthropic opportunities to support the health care system.
Alan Butler, CoxHealth’s system director of public safety and security, said in a statement on September 17 that “panic buttons fill a critical void.”
“Personal Panic Buttons are one more tool in the battle to keep our staff safe and further demonstrate this organization’s commitment to maintaining a safe work and care environment,” he said.
The panic buttons are being implemented following an increased year of violence for health care workers. Patient assaults on Cox Medical Center Branson staff members have tripled in the past year, according to the facility.
The number of workplace assaults increased from 40 incidents in 2019 to 123 in 2020, the foundation said, citing the medical center’s data; the number of injuries during that time increased from 17 to 78.
But even those numbers may not paint the full picture.
Angie Smith, the medical center’s patient safety facilitator, said that many workplace violence events go underreported because “staff don’t feel like they would be supported or don’t feel like they would be able to do anything about it.”
“The biggest part of being in health care now is not only being able to give excellent care to your patient you’ve been assigned and to make them feel safe,” she said, “but to also feel safe yourself as their primary caregiver.”
Workplace violence in medical facilities was a “serious problem” even before the pandemic, according to the Occupational Safety and Health Administration. From 2002 to 2013, incidents of “serious” violence, which required the injured person to take days off to recover, was four times more common in health care than in private industries.
A 2018 survey of 3,539 emergency physicians by the American College of Emergency Physicians found that nearly half of participants have been assaulted while working in the emergency department. Roughly 97% of those assaults were committed by patients.
https://www.cbsnews.com/news/health-care-workers-missouri-covid-attacks-panic-buttons/





More Stories
Amid nationwide psychological well being crisis, suicide prevention hotlines battle with repeat callers
California regulation aims to force people today with psychological disease to get assistance
California is initial condition to ban 4 food items additives for most cancers, other well being challenges : NPR